- Apr 13, 2026
- By TJICLondon
Arthrosamid for Knee Osteoarthritis: Evidence, Outcomes and How It Compares to Other Treatments
Living with Knee Osteoarthritis: When Conservative Treatment Is No Longer Enough
Knee osteoarthritis is one of the most common musculoskeletal conditions seen at Joint Care London. It affects millions of people in the UK, and for many patients, it quietly reshapes daily life long before a formal diagnosis is made. The morning stiffness that takes twenty minutes to ease. The hesitation before climbing stairs. The moment you start avoiding walks you used to enjoy. These are the early signals that the cartilage cushioning your knee joint is beginning to break down.
For most people, the first line of management involves weight optimisation, targeted physiotherapy, and activity modification. These remain cornerstones of treatment, and for knee osteoarthritis in its earlier stages, they can make a significant difference. But there comes a point for many patients where conservative measures alone are no longer providing adequate relief, and the question shifts from "how do I manage this?" to "what are my actual options?"
This is where injectable treatments have an increasingly important role to play — and Arthrosamid in particular has emerged as one of the most significant advances in non-surgical knee treatment in recent years.
What Is Arthrosamid?
Arthrosamid is a non-degradable polyacrylamide hydrogel — a soft, gel-like substance that is injected directly into the knee joint as a single-dose treatment. The term "hydrogel" simply means it is a gel that contains a very high proportion of water. In fact, Arthrosamid is 97.5% water, with a 2.5% cross-linked polyacrylamide backbone that gives it structure and stability.
What makes Arthrosamid different from other knee joint injections is what happens after it is administered. Rather than simply supplementing the joint fluid and being gradually absorbed over weeks or months, Arthrosamid integrates with the synovial membrane — the inner lining of the knee joint. Once embedded there, it acts as a permanent cushioning layer within the joint itself, helping to reduce pain, improve joint lubrication, and protect the remaining cartilage from further mechanical stress.
The polyacrylamide material is not new — it has been used safely in medical applications for over two decades. But its application as an intra-articular injection for knee osteoarthritis, under the brand name Arthrosamid, represents a more recent and carefully developed use of the technology. You can read more about the full treatment process, post-procedure guidance, and safety profile on our dedicated Arthrosamid treatment page.
Who Is Arthrosamid Suitable For?
Arthrosamid is designed for patients with mild to moderate knee osteoarthritis who are experiencing persistent pain and stiffness despite trying conservative measures. It tends to be most appropriate for patients who:
- Have confirmed knee osteoarthritis on imaging (X-ray or MRI), typically Grade 2 or Grade 3 on the Kellgren-Lawrence scale
- Have not achieved adequate or sustained relief from physiotherapy, oral anti-inflammatories, or supplements
- Have had short-lived benefit from steroid or hyaluronic acid injections and are looking for a longer-lasting alternative
- Want to delay or avoid knee replacement surgery
- Are not yet at a stage where surgical intervention is clinically indicated or personally desired
Arthrosamid is not typically recommended for patients with severe end-stage arthritis where there is very little joint space remaining — in those cases, the structural changes within the joint may be too advanced for an injection-based approach to provide meaningful benefit. During your consultation at Joint Care London, our specialist will review your imaging and clinical history to determine whether Arthrosamid is likely to be the right fit for you.
A Note on Age and Activity Level
One question patients frequently ask is whether Arthrosamid is suitable for active people who want to stay that way. The answer is generally yes. Many patients who come to us for Arthrosamid are in their 50s, 60s, or 70s and are keen to continue walking, cycling, swimming, or playing golf — activities that are genuinely beneficial for joint health but difficult to sustain when knee pain is limiting them. Arthrosamid's aim is precisely to restore that quality of life, keeping patients active without the recovery and rehabilitation demands of surgery.
How Does Arthrosamid Relieve Knee Pain?
To understand how Arthrosamid works, it helps to understand what goes wrong in knee osteoarthritis in the first place.
Healthy cartilage acts as a shock absorber within the knee, distributing load across the joint surface and allowing the bones to glide smoothly against one another. The knee joint is also lined by the synovial membrane, which produces synovial fluid — the joint's natural lubricant. In osteoarthritis, cartilage progressively thins and breaks down. The synovial fluid changes in composition and loses some of its protective properties. The result is a joint that is less well-cushioned, less well-lubricated, and more prone to inflammation — which is what causes the pain, swelling, and stiffness that patients experience.
When Arthrosamid is injected into the joint, the hydrogel integrates with the synovial membrane and remains there. It creates a stable, cushioning presence within the joint lining that helps to:
- Reduce the mechanical stress transmitted through the joint with every step
- Improve load distribution across the joint surface
- Restore a more protective environment within the joint, reducing the inflammatory signals that drive pain
- Improve the overall function and comfort of the knee during everyday activities
Critically, because Arthrosamid is non-degradable, it does not break down and get absorbed the way hyaluronic acid does. The cushioning effect is intended to be lasting — which is what distinguishes it from other intra-articular injection options and gives it its potential for longer-term pain relief.
What Does the Clinical Evidence Show?
Arthrosamid has been the subject of several clinical trials, the most significant of which is the TACIT trial — a multicentre, randomised controlled trial conducted in Denmark and published in peer-reviewed literature. This is the gold standard of clinical evidence, comparing patients treated with Arthrosamid against a control group.
The key findings from the TACIT trial and subsequent follow-up data are encouraging:
- Patients treated with Arthrosamid reported statistically significant reductions in pain and improvement in knee function compared to controls
- The treatment demonstrated a strong safety profile, with no serious adverse events directly attributable to the hydrogel itself
- Improvements in pain and function were sustained at two and three years of follow-up in a substantial proportion of patients
- At Joint Care London, clinical outcomes are consistent with published data: approximately 15–50% of patients experience very significant improvement, 70–75% report good improvement overall, and around 5–10% notice minimal change
It is worth being honest about what "improvement" means in this context. Arthrosamid is not a cure for osteoarthritis — the underlying joint disease does not reverse. What it can do, for the majority of patients, is meaningfully reduce the daily pain and stiffness that limits their activity, and in many cases provide that relief for considerably longer than other injectable options. For patients who have been cycling through six-monthly steroid injections with diminishing returns, that distinction matters enormously.
How Does Arthrosamid Compare to Other Knee Injection Treatments?
Patients considering Arthrosamid often want to understand how it compares to the other injection options available for knee osteoarthritis. The honest answer is that different treatments suit different patients at different stages of the condition — and the best approach is always guided by a thorough consultation rather than a one-size-fits-all protocol.
Arthrosamid vs. Steroid Injections
Corticosteroid injections are among the most commonly used treatments for knee arthritis pain. They work by delivering a powerful anti-inflammatory agent directly into the joint, which can provide rapid and significant pain relief — often within 24 to 48 hours. For acute flare-ups of knee pain or for patients who need fast relief before an important event, they can be highly effective.
The limitation is duration. Steroid injections typically provide relief for a period of weeks to months — in good responders, perhaps up to six months — but the effect diminishes with repeated use, and there are clinical guidelines around how frequently they should be administered in the same joint. Repeated high-dose steroid injections can also have a mild catabolic effect on joint tissues over time, which is a consideration for younger, more active patients.
Arthrosamid, by contrast, is a single injection. It does not work as quickly — most patients begin noticing improvement from around four weeks post-injection — but the potential duration of benefit is considerably longer, with effects reported to last up to three years. For patients who are looking for sustained relief rather than acute management, this is a meaningful difference.
Arthrosamid vs. Hyaluronic Acid Injections
Hyaluronic acid (HA) injections, also known as viscosupplementation, work by supplementing the natural hyaluronan in the joint fluid, improving lubrication and reducing friction. They are generally well-tolerated and can provide good relief for mild to moderate osteoarthritis, typically lasting three to six months or longer in some patients.
Hyaluronic acid is, however, gradually broken down and absorbed by the body. This means the treatment needs to be repeated periodically to maintain its effects. Arthrosamid's non-degradable nature means it is not subject to the same degradation — once integrated into the synovial membrane, it remains there. For patients who find that hyaluronic acid injections provide good but short-lived benefit, Arthrosamid may offer a more durable solution without the need for repeated procedures.
Arthrosamid vs. Platelet-Rich Plasma (PRP)
Platelet-rich plasma (PRP) injections involve taking a small sample of the patient's own blood, centrifuging it to concentrate the growth factors within the platelets, and injecting this back into the affected joint. PRP has good evidence particularly for early-stage knee arthritis and for certain tendon conditions, and because it uses the patient's own biological material, it has an excellent tolerability profile.
PRP works through a different mechanism — it aims to harness the body's own healing and regenerative signals to modify the joint environment over time. It tends to be most effective in earlier-stage disease. Arthrosamid, on the other hand, is a mechanical intervention — it works by physically integrating with the joint lining to provide cushioning and reduce load. The two approaches are not mutually exclusive, and in some cases a combination may be considered, though this would always be discussed individually.
Arthrosamid vs. Knee Replacement Surgery
This is, for many patients, the question that brings them to our clinic in the first place: "Can I avoid a knee replacement?"
Knee replacement surgery is a very effective procedure for end-stage osteoarthritis with severe structural damage, and for the right patients it can be transformative. But it is also major surgery, with a recovery period typically measured in months, and with associated risks that include infection, blood clots, and the possibility that the implant may need revision over time.
Arthrosamid is not a competitor to knee replacement for patients who genuinely need surgery. What it can do is provide significant relief for patients who are not yet at that stage — effectively buying time, sometimes years of good-quality active life, before surgery becomes necessary. For some patients, particularly older or frailer individuals for whom surgery carries higher risk, it may provide meaningful long-term management without the need for surgery at all.
What Can Patients Realistically Expect?
The Timeline
Arthrosamid works gradually. Unlike a steroid injection, which can provide noticeable relief within days, the hydrogel needs time to integrate with the synovial membrane and for the joint to respond. Most patients begin to notice a meaningful difference at around the four-week mark, with continued gradual improvement over the following weeks and months.
The Duration
Clinical data supports the potential for Arthrosamid to provide pain relief for up to three years in good responders. This is not a guarantee — individual responses vary, and a proportion of patients will experience shorter-lasting benefit. That said, even for patients who fall outside the strongest responder group, a year or more of meaningful pain relief from a single injection represents a very worthwhile outcome.
Can the Injection Be Repeated?
Because Arthrosamid is non-degradable and integrates with the joint lining, the question of re-injection is handled differently to hyaluronic acid. If a patient had a good initial response and finds that the benefit diminishes after a number of years, there is evidence that a repeat injection can be considered. This would be assessed on a case-by-case basis during a follow-up consultation.
The Role of Ultrasound Guidance
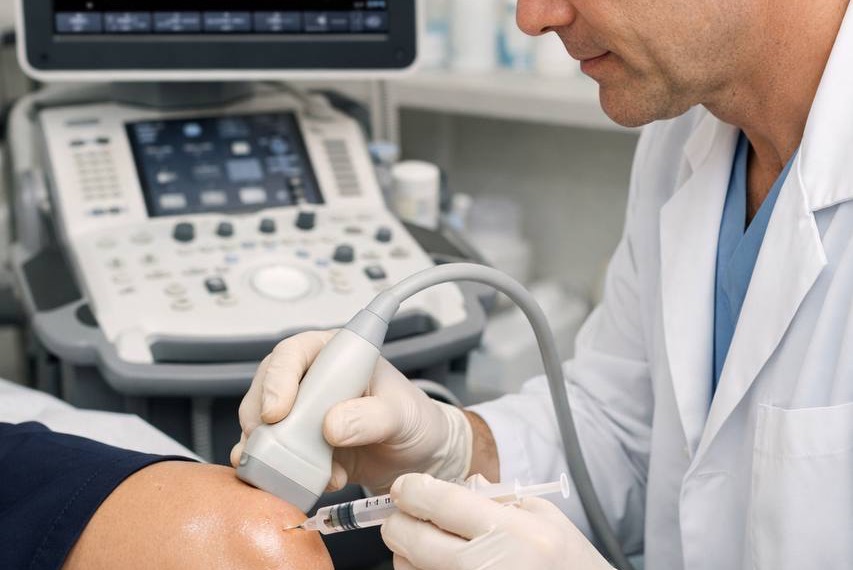
All Arthrosamid injections at Joint Care London are performed under ultrasound guidance by experienced consultant musculoskeletal doctors. Ultrasound guidance is not a cosmetic addition to the procedure — it is clinically important. Accurate placement of the hydrogel within the joint space is essential for it to work as intended.
Ultrasound guidance also allows the clinician to aspirate any excess fluid from the joint before the Arthrosamid is administered. In an arthritic knee that has accumulated inflammatory fluid — a common finding — this drainage step is itself often immediately relieving, and creates the optimal environment for the hydrogel to integrate effectively.
Knee Osteoarthritis and Quality of Life: The Bigger Picture
It is easy to focus on pain scores and clinical outcomes when discussing any treatment for knee arthritis, but the impact of persistent knee pain on quality of life is more far-reaching than a number on a scale suggests. Chronic joint pain disrupts sleep. It limits participation in activities that bring people joy and connection — sport, travel, gardening, playing with grandchildren. It can contribute to low mood and social withdrawal. And in many cases, it creates a cycle of reduced activity that leads to muscle weakening around the knee, which in turn accelerates joint deterioration.
Effective knee pain relief is not just about the joint — it is about enabling people to live the lives they want to live. That is the lens through which we approach treatment decisions at Joint Care London, and it is the lens through which Arthrosamid's benefits should be understood.
If you are living with knee osteoarthritis symptoms and want to understand whether Arthrosamid or another injection approach might be right for you, the first step is a consultation with one of our specialists. We will review your history, your imaging, your previous treatment responses, and your goals — and give you an honest, evidence-based assessment of your options. Call us on 0333 011 1885 or book online to arrange an appointment at our clinic in London.