- Nov 12, 2025
- By TJICLondon
Hip Osteoarthritis Treatment: Non-Surgical Options Explained
Hip Osteoarthritis Treatment: Your Guide to Non-Surgical Options
If you have been told you have hip osteoarthritis, or if you have been living with deepening groin pain, stiffness first thing in the morning, or a nagging ache that stops you doing the things you love, you are far from alone. Hip osteoarthritis affects millions of people in the UK, and for many it becomes a significant barrier to daily life long before surgery ever becomes necessary. The good news is that there is a broad spectrum of effective hip osteoarthritis treatment options available — and most people can reduce their pain and protect their quality of life without going under the knife.
At Joint Care London, our specialist team focuses exclusively on musculoskeletal conditions. We work with patients across London to create personalised, evidence-based treatment plans that keep them mobile, comfortable, and in control of their own care. This guide explains everything you need to know about hip osteoarthritis — what it is, how it progresses, and which treatments are most likely to help.
What Is Hip Osteoarthritis?
Osteoarthritis (OA) is the most common form of arthritis. It is a condition affecting the cartilage — the smooth, protective tissue that cushions the ends of the bones inside a joint. In a healthy hip, cartilage allows the ball of the femur (thigh bone) to glide effortlessly within the cup-shaped socket of the pelvis. Over time, with osteoarthritis, this cartilage gradually breaks down. As it thins and roughens, the bones begin to move with more friction, the joint can become inflamed, and in advanced cases bone may rub directly against bone.
The hip is a large, load-bearing joint that supports the full weight of the body during almost every activity — walking, climbing stairs, getting out of a chair, even standing still. This makes it particularly vulnerable to the wear and tear process that drives osteoarthritis. You can read more about the condition on our dedicated hip osteoarthritis conditions page.
Who Gets Hip Osteoarthritis?
- Age: The risk increases significantly after 45, and more so after 60.
- Previous joint injury: A hip fracture, dislocation, or sports injury can accelerate cartilage breakdown years or even decades later.
- Hip dysplasia: A condition where the hip socket is abnormally shallow, placing uneven stress on the cartilage.
- Obesity: Excess body weight multiplies the load through the joint with every step.
- Occupation and activity: Jobs or sports involving heavy lifting, repetitive movements, or prolonged standing carry higher risk.
- Family history: A genetic predisposition can make you more susceptible.
Recognising Hip Osteoarthritis Symptoms
- A deep, aching pain in the groin, inner thigh, or buttock — pain that may also radiate down to the knee
- Stiffness after rest, particularly on waking in the morning or after sitting for a long time
- Reduced range of movement — difficulty putting on socks and shoes, getting in and out of a car, or climbing stairs
- A grinding, clicking, or grating sensation within the joint (known as crepitus)
- Pain that worsens with activity and eases with rest (though in later stages it may become constant)
- A tendency to limp or shift weight to the opposite side to reduce discomfort
How Hip Osteoarthritis Progresses
OA is broadly classified into stages, from mild (minor cartilage roughening with minimal symptoms) through moderate (noticeable cartilage loss, regular pain, and reduced mobility) to severe (significant bone-on-bone contact, constant pain, and substantial functional limitation). Progression is not inevitable or uniform — many people remain at a mild or moderate stage for years, particularly with appropriate treatment and lifestyle measures.
Getting a Diagnosis
A thorough clinical assessment is the foundation of any effective treatment plan. Diagnosis typically involves a detailed history of your symptoms, a physical examination to assess your range of movement and identify where the pain originates, and imaging — most commonly X-ray, which reveals the degree of joint space narrowing and any bony changes. An MRI scan may be requested when the picture is less clear, or when other causes of hip pain need to be excluded.
Conservative Management: The Essential Foundation
Exercise and Physiotherapy
Strengthening the muscles around the hip — particularly the glutes, hip abductors, and core — reduces the load placed on the joint and improves stability. Low-impact aerobic activity such as swimming, cycling, and walking also helps maintain joint health and manage weight. A physiotherapist can design a programme tailored to your current level of function and progression goals.
Weight Management
For every kilogram of body weight lost, the force through the hip joint reduces by approximately three to six kilograms with each step. Even modest weight loss can produce meaningful reductions in pain and slow the rate of cartilage breakdown.
Activity Modification and Pacing
Learning to balance activity with rest, avoid high-impact loading during flare-ups, and use supportive footwear or a walking aid when needed can all help manage day-to-day symptoms without restricting your life unnecessarily.
Oral Analgesics and Anti-Inflammatories
Paracetamol, topical NSAIDs, and oral NSAIDs such as ibuprofen or naproxen can provide useful short-term pain relief. However, long-term use of oral NSAIDs carries risks — particularly for the stomach and cardiovascular system — that need careful consideration.
Injection Options for Hip Osteoarthritis
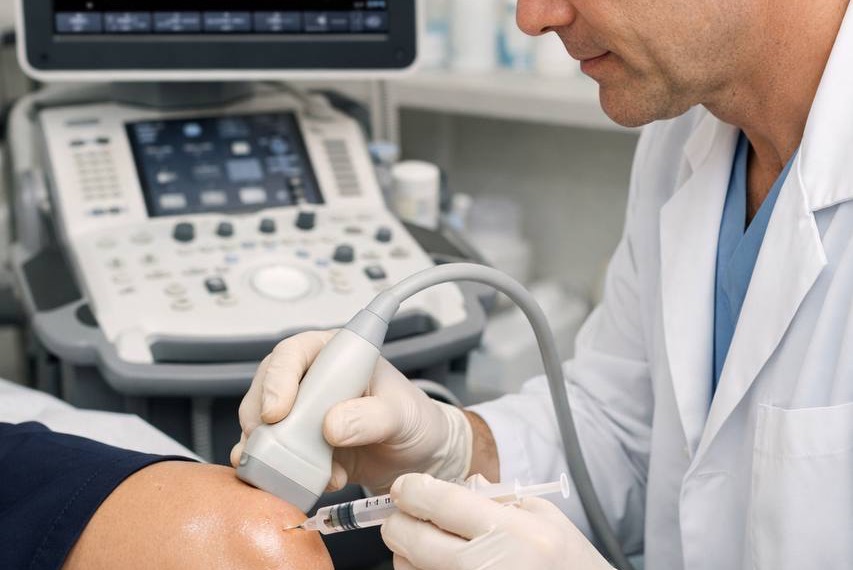
When conservative measures are insufficient to control pain and maintain function, image-guided injections into the hip joint offer a targeted, minimally invasive route to relief. At Joint Care London, all hip injections are performed under ultrasound or fluoroscopic guidance to ensure precision and safety.
Corticosteroid (Steroid) Injections
A steroid injection into the hip combines a corticosteroid with a local anaesthetic. By delivering the anti-inflammatory agent directly into the joint space, it reduces the inflammation that drives pain far more effectively — and with far fewer systemic side effects — than oral medication can achieve.
Most patients notice significant improvement within a few days of the injection, with pain relief typically lasting between six weeks and six months. Learn more on our steroid injections page.
Hyaluronic Acid Injections (Viscosupplementation)
Hyaluronic acid is a substance that occurs naturally in healthy joint fluid, acting as both a lubricant and a shock absorber. Hyaluronic acid hip injections replenish this depleted supply, restoring some of the joint's natural cushioning properties. Results tend to develop more gradually than with steroids but the duration of benefit is often longer, with many patients reporting relief for six months to a year or more. Find out more on our hyaluronic acid injections page.
Platelet-Rich Plasma (PRP) Injections
Platelet-rich plasma (PRP) is a regenerative treatment prepared from a small sample of the patient's own blood. The concentrated plasma, rich in growth factors, is then injected into the hip joint to stimulate the joint's own repair processes and reduce inflammation. Because PRP is derived from the patient's own blood, the risk of allergic reaction or rejection is negligible. Read more on our platelet-rich plasma injections page.
Arthrosamid: A Longer-Term Hip Replacement Alternative
Arthrosamid is a polyacrylamide hydrogel injected directly into the hip joint. Unlike steroid or hyaluronic acid injections, Arthrosamid is not absorbed or broken down by the body. It integrates with the soft tissue inside the joint capsule, forming a stable, lasting cushion that restores the joint's internal environment and reduces the friction and inflammation that cause pain.
For patients with moderate to severe hip osteoarthritis who want to delay or avoid hip replacement, Arthrosamid represents a genuinely compelling hip replacement alternative with clinical data demonstrating sustained pain relief over two years and beyond. Find out more on our dedicated Arthrosamid page.
What to Expect From Your Treatment Journey
- Initial consultation: A detailed review of your history, symptoms, and any existing imaging, followed by a physical examination.
- Diagnosis and discussion: We will explain what is happening in your joint in plain language and discuss the full range of relevant treatment options.
- Treatment: All hip joint injections are performed under image guidance by our specialist team on an outpatient basis.
- Follow-up: We monitor your response and adjust the plan as needed.
When Should You Consider Hip Replacement Surgery?
Surgery is not the enemy — for some patients with severe, end-stage osteoarthritis, total hip replacement is the right choice. However, it is major surgery with a substantial recovery period. The general indicators for considering surgical referral include severe constant pain no longer controlled by conservative treatment, profound loss of function, and advanced radiological changes consistent with near-complete cartilage loss.
For everyone else, the goal is to maximise function and quality of life with the least invasive interventions possible. Modern injection treatments, particularly newer options like Arthrosamid, have extended the window during which surgery can be responsibly deferred for many patients.
Living Well With Hip Osteoarthritis
A diagnosis of hip osteoarthritis does not have to mean a progressive decline into immobility. With the right combination of exercise, lifestyle management, and appropriately targeted injection treatment, most patients are able to maintain an active, fulfilling life.
The key is not to delay. Pain that is left untreated tends to lead to guarding, muscle weakness, reduced activity, weight gain, and worsening joint function — a cycle that is much harder to reverse the longer it continues. If you are experiencing hip pain in London and think osteoarthritis may be the cause, seeking an early, specialist opinion is the single most important step you can take.