- Jan 15, 2026
- By TJICLondon
PRP Injection: What It Is, How It Works, and What to Expect
If you have been living with persistent joint pain, a nagging tendon injury that simply will not heal, or the gradual stiffness of osteoarthritis, you may have come across the term PRP injection — and wondered whether it could help you. Platelet rich plasma therapy has attracted considerable attention over the past decade, both in professional sport and in everyday clinical practice. At Joint Care London, we offer PRP as part of a broader menu of evidence-based platelet rich plasma injections for patients across London seeking a non-surgical route to lasting relief.
This guide explains exactly what PRP is, how it is prepared, which conditions it is best suited to, and what you can realistically expect from treatment — so you can make a well-informed decision about your care.
What Is a PRP Injection?
PRP stands for platelet rich plasma. It is a regenerative injection therapy that uses components drawn from your own blood to encourage the body's natural healing processes at the site of injury or degeneration.
Blood is made up of several elements: red blood cells, white blood cells, plasma (the liquid carrier), and platelets. Platelets are tiny cell fragments best known for their role in clotting, but they also contain a dense store of growth factors — signalling proteins that orchestrate tissue repair. Platelet rich plasma is simply plasma in which the concentration of platelets has been significantly increased above baseline levels, typically by a factor of three to five times.
Because PRP is derived from your own blood, there is no risk of allergic reaction or tissue rejection. This makes it a very well-tolerated treatment with a strong safety profile.
How Is PRP Prepared?
The preparation process is straightforward and takes place in the clinic on the day of your appointment.
- Blood draw: A small volume of blood — usually around 15–30 ml, less than a standard blood donation — is taken from a vein in your arm.
- Centrifugation: The blood sample is placed into a medical centrifuge, a machine that spins at high speed to separate its components by density. This process typically takes around 10–15 minutes.
- Extraction: The platelet-rich layer is carefully drawn off and prepared for injection. Depending on the system used, white blood cells may be included or excluded — a distinction that matters clinically for certain conditions.
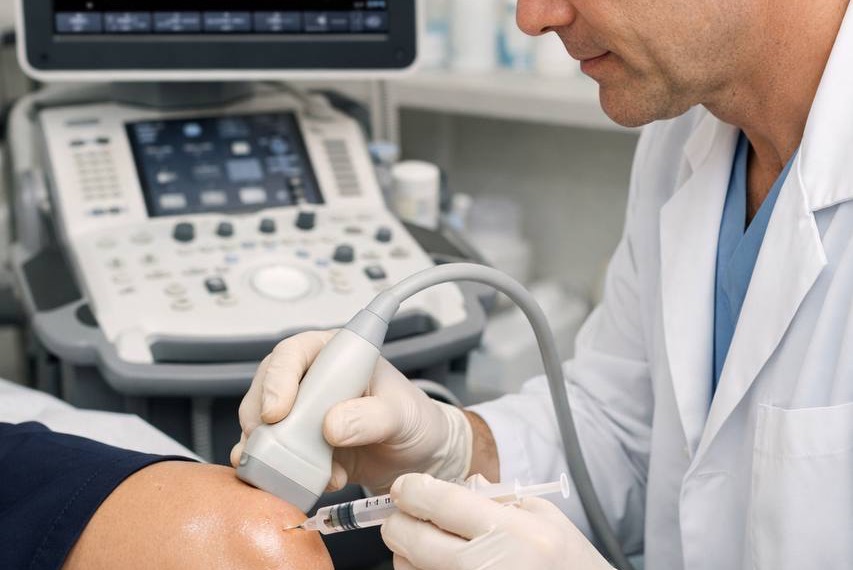
- Injection: The concentrated platelet rich plasma is injected precisely into the affected area, usually under ultrasound guidance to ensure accuracy.
The entire appointment, from blood draw to injection, typically takes around 45 to 60 minutes. Because PRP is autologous — meaning it comes from your own body — no pre-screening for compatibility is required.
How Does PRP Work?
When platelets are activated at the injection site, they release their stored growth factors. These include substances such as platelet-derived growth factor (PDGF), transforming growth factor-beta (TGF-β), and vascular endothelial growth factor (VEGF). In plain terms, these are molecular signals that tell surrounding cells to begin repairing and regenerating damaged tissue.
The key mechanisms that make a PRP injection useful in musculoskeletal medicine include:
- Stimulation of collagen synthesis — important for tendon and ligament healing
- Promotion of cartilage cell (chondrocyte) activity — relevant in osteoarthritic joints
- Modulation of inflammation — reducing the chronic, destructive inflammation seen in tendinopathy and joint degeneration
- Improved blood supply — encouraging new vessel formation to support tissue repair
Crucially, PRP is not simply a pain-masking treatment. Unlike a corticosteroid, which suppresses inflammation broadly, PRP aims to address the underlying biological environment that is preventing healing from occurring naturally. This is why it is classified as a regenerative injection therapy.
What Conditions Can PRP Treat?
PRP for joints and soft tissues has a growing evidence base, and our clinicians at Joint Care London use it selectively where the research supports meaningful benefit.
Knee Conditions
PRP knee treatment is one of the most studied applications of this therapy. It is particularly well evidenced in knee osteoarthritis, where randomised controlled trials have shown meaningful improvements in pain and function — especially in mild to moderate disease. PRP has also been used effectively for knee ligament injuries and post-surgical recovery support.
Shoulder Conditions
PRP shoulder injections are commonly used for rotator cuff tendinopathy, partial rotator cuff tears, and chronic shoulder pain that has not responded to physiotherapy alone. The shoulder is a complex joint and accurate, ultrasound-guided delivery is essential for good outcomes in this region.
Tendon and Ligament Injuries
PRP tendon treatment is one of the original and best-supported uses of this therapy. Conditions where tendon healing has stalled — a state known as tendinopathy — respond well to the growth factor stimulus PRP provides. Common examples include:
- Achilles tendinopathy
- Patellar tendinopathy (jumper's knee)
- Lateral epicondylalgia (tennis elbow)
- Gluteal tendinopathy
- Hamstring tendinopathy
- Plantar fasciitis
Other Joints
Beyond the knee and shoulder, PRP is used at Joint Care London for hip joint pain, ankle arthritis, and thumb base (carpometacarpal) osteoarthritis, among other presentations. Each case is assessed individually to confirm that PRP is the most appropriate option.
PRP Versus Steroid Versus Hyaluronic Acid: Understanding Your Options
Patients frequently ask how a PRP injection compares with other available treatments. The honest answer is that each has a different mechanism, a different evidence base, and suits different clinical scenarios. There is rarely a single "best" option — it depends on your diagnosis, disease stage, and treatment goals.
PRP vs Corticosteroid Injections
Steroid injections (corticosteroids) are highly effective at rapidly reducing inflammation and providing short-term pain relief — often within days. They are a well-established, lower-cost option and are particularly useful when rapid symptom control is the priority, for example before a planned event or to enable participation in rehabilitation.
However, repeated steroid injections can weaken tendons and cartilage over time, and their effect is generally short to medium term. PRP, by contrast, targets the healing process itself and may offer longer-lasting benefit — though it typically takes several weeks for the full effect to develop. For tendon conditions in particular, current evidence suggests PRP may produce more durable outcomes than steroid over the longer term.
PRP vs Hyaluronic Acid Injections
Hyaluronic acid (HA) injections — sometimes called viscosupplementation — work by supplementing the natural lubricating fluid within a joint, reducing friction and providing a cushioning effect. They are most commonly used in knee osteoarthritis.
Both PRP and HA have good evidence in knee osteoarthritis, and some studies suggest PRP produces superior results particularly in younger patients and those with less severe disease. The two treatments are not mutually exclusive; in certain cases, combining approaches or sequencing them can be clinically appropriate.
What About Arthrosamid?
For patients with moderate to severe knee osteoarthritis where longer-term joint support is a priority, Arthrosamid — a polyacrylamide hydrogel injection — offers a durable single-treatment option. Your clinician will explain how this fits alongside PRP as part of a considered treatment plan.
What to Expect: Procedure and Recovery Timeline
Before Your Appointment
In the days before your PRP injection, you will be advised to avoid non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or naproxen, as these can reduce platelet activity and potentially diminish the treatment effect. Your clinician will give you specific guidance at the point of booking.
You do not need to fast. Staying well hydrated before your appointment helps make the blood draw straightforward.
On the Day
The appointment proceeds as described above — blood draw, centrifugation, and injection. Most patients find the injection itself no more uncomfortable than a standard joint injection. Ultrasound guidance is used to ensure the PRP is delivered precisely to the target tissue.
You will be able to leave the clinic under your own steam. We recommend arranging transport rather than driving yourself, particularly for lower limb injections.
The Days Following Injection
It is entirely normal to experience a temporary post-injection flare — an increase in soreness and swelling at the treated site — for two to five days after the procedure. This is not a sign that something has gone wrong; it reflects the inflammatory response that PRP intentionally initiates as part of the healing process. Avoid NSAIDs during this period. Paracetamol can be taken for comfort if needed.
We advise relative rest of the treated area for the first one to two weeks, followed by a graded return to activity and exercise — ideally in conjunction with physiotherapy.
When Will I See Results?
- Weeks 1–4: Some patients notice a gradual easing of symptoms. Others may feel little change yet.
- Weeks 6–12: This is typically when the most meaningful improvement becomes apparent as tissue remodelling progresses.
- 3–6 months: The full benefit of a PRP course is usually realised within this window.
Many patients receive a course of two to three injections spaced four to six weeks apart, particularly for joint conditions. Your clinician will advise on the optimal protocol for your specific situation.
Who Is a Good Candidate for PRP?
- You have a confirmed musculoskeletal diagnosis — osteoarthritis, tendinopathy, or a soft tissue injury — where conservative measures have been tried
- You wish to explore a regenerative approach before considering surgery
- You have had limited or short-lived benefit from previous steroid injections
- You are in generally good health with no active infection, clotting disorder, or blood malignancy
- You understand that improvement is gradual and are committed to a rehabilitation programme alongside treatment
PRP is generally not recommended during pregnancy, for patients on anticoagulant medication, or where there is active systemic inflammatory disease requiring different management. A full medical history is taken at consultation to confirm suitability.
Realistic Outcomes: What PRP Can and Cannot Do
Evidence for PRP is consistently positive across several musculoskeletal conditions, particularly knee osteoarthritis and tendinopathy. Many patients experience significant, sustained reductions in pain and meaningful improvements in function — allowing them to return to activities that joint pain had previously curtailed.
That said, PRP is not a cure for structural degeneration. It cannot reverse severe joint destruction or regrow tissue that is entirely absent. Results vary between individuals, and a small proportion of patients do not respond. The aim is to create a more favourable biological environment for healing and to reduce pain and improve function in a durable way.
At Joint Care London, we believe in honest, evidence-based conversations with every patient. If PRP is not the right option for you, we will say so — and discuss what alternatives may be more suitable for your specific condition and goals.
If you would like to find out whether a PRP injection could be right for you, we welcome you to book a consultation at our clinic in London. Our specialists will carry out a thorough assessment, review any available imaging, and work with you to build a personalised joint pain treatment plan.