- Jul 02, 2025
- By TJICLondon
Plantar Fasciitis Treatment London | Heel Pain Injections
If you have landed on this page, there is a reasonable chance you have already tried rest, new shoes, stretching exercises, and perhaps a course of physiotherapy — and your heel still hurts. Plantar fasciitis is one of the most common causes of foot pain in adults, yet it is also one of the most stubbornly persistent. Understanding why it behaves the way it does, and what treatments are actually available, is the first step toward lasting relief.
At Joint Care London, we work with patients who have often exhausted first-line options and are looking for a clearer path forward. This guide walks you through the condition itself, the evidence behind each treatment approach, and what to realistically expect from injection-based care.
What Is Plantar Fasciitis?
The plantar fascia is a thick band of connective tissue running along the sole of your foot, connecting your heel bone (calcaneus) to the base of your toes. Its job is to support the arch of the foot and absorb the mechanical load of walking, running, and standing.
Plantar fasciitis occurs when this tissue becomes irritated, usually at the point where it attaches to the heel bone. The term is widely used, though clinicians now recognise that in many chronic cases the problem is less about active inflammation and more about a degenerative process within the tissue itself. This distinction matters, because it influences which treatments are most likely to work.
Why Is Plantar Fasciitis So Persistent? The Biology Explained
Unlike muscle, the plantar fascia has a relatively poor blood supply. This means that when micro-tears or degenerative changes occur, the body's natural repair process is slow and often incomplete. Instead of laying down healthy collagen, the tissue can enter a cycle of failed healing — a process sometimes referred to as fasciopathy.
Repetitive loading continues to stress tissue that has not fully healed. Without interrupting that cycle, symptoms can persist for twelve months or longer, even with diligent conservative care.
Symptoms and Diagnosis
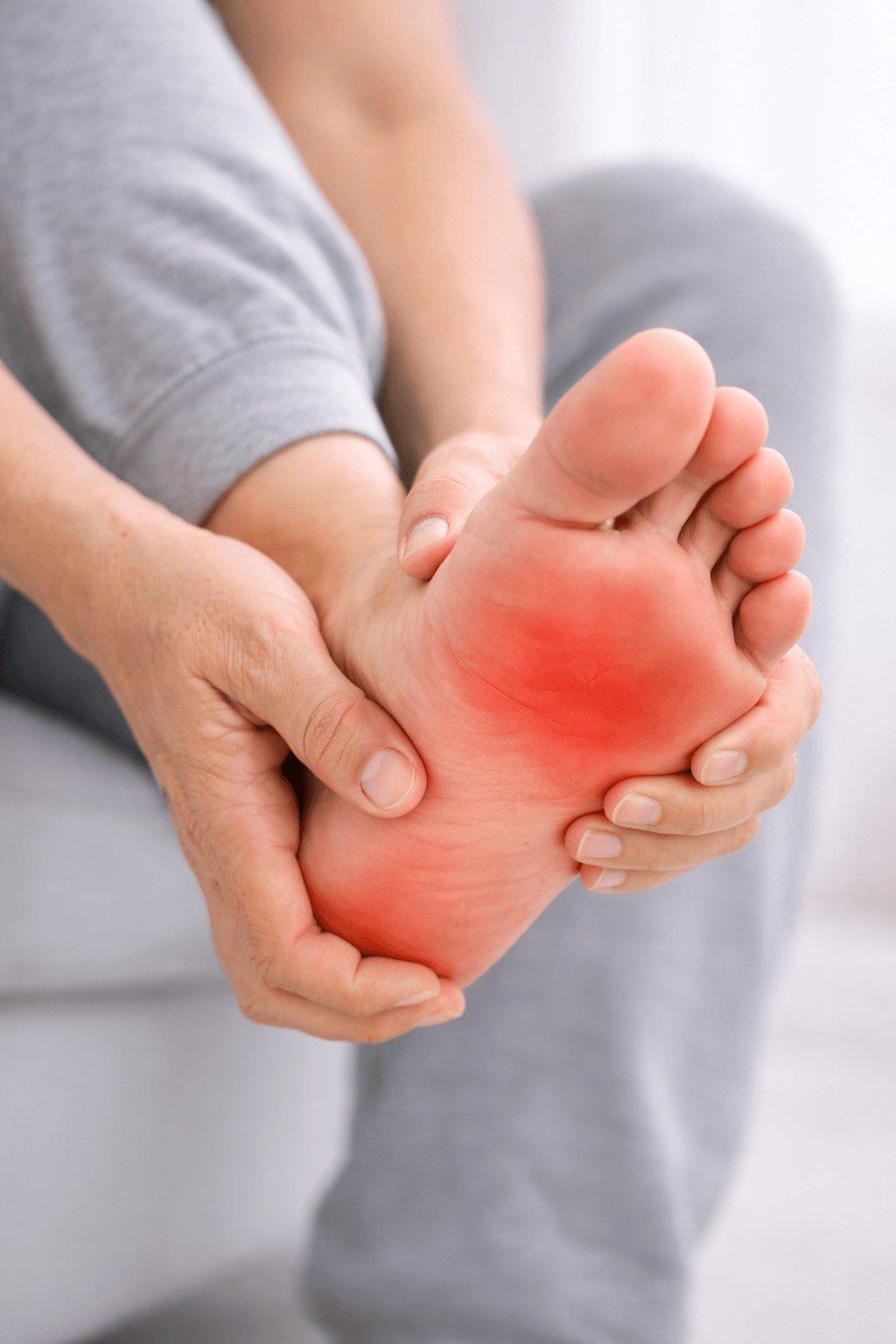
The hallmark symptom is a sharp, stabbing pain at the base of the heel, typically worst with the first steps in the morning or after a period of sitting. This start-up pain often eases after a few minutes of walking, only to return after prolonged activity or at the end of the day.
Common associated symptoms include:
- Tenderness directly over the heel, particularly on the inner (medial) side
- Tightness in the calf and Achilles tendon
- Aching along the arch of the foot
- Worsening pain after — rather than during — exercise
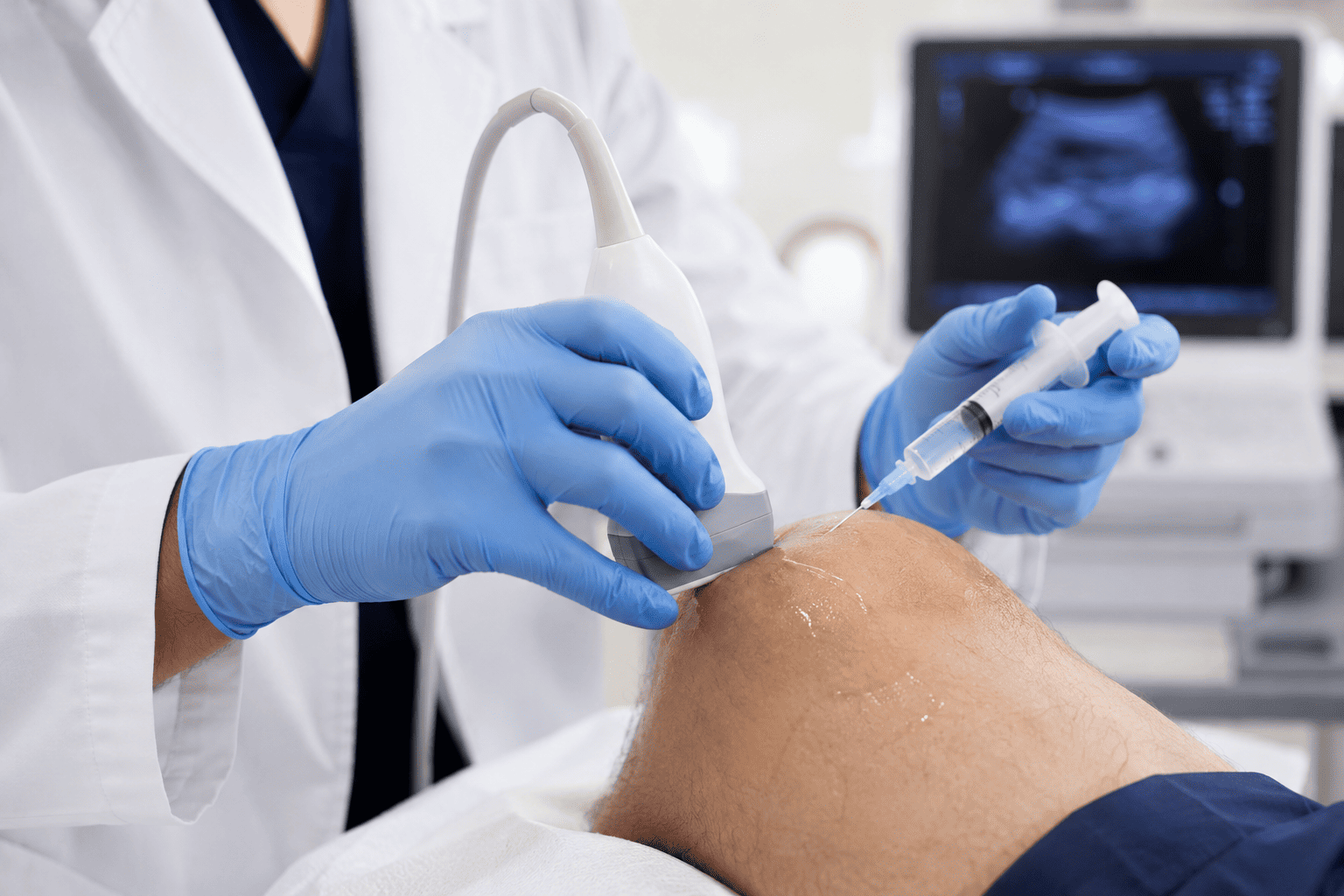
Diagnosis is primarily clinical, based on your history and a physical examination. In persistent or atypical cases, diagnostic ultrasound is a valuable tool. It can visualise thickening of the fascia, identify micro-tears, and confirm the exact location of pathology.
Conservative Treatment: The Essential First Step
Stretching and Eccentric Exercise
Targeted stretching of the plantar fascia and calf muscles reduces tensile load on the heel attachment. A physiotherapist can design a specific programme; consistency over several weeks is key.
Footwear and Orthotics
Supportive footwear with adequate arch support and cushioning reduces mechanical stress. Avoiding walking barefoot on hard floors, particularly first thing in the morning, makes a meaningful difference for many patients.
Load Management
Temporarily reducing high-impact activities while maintaining lower-impact movement such as swimming or cycling helps prevent ongoing tissue damage without complete rest.
Shockwave Therapy
Extracorporeal shockwave therapy (ESWT) uses acoustic energy to stimulate tissue repair and is supported by good evidence for chronic plantar fasciitis. It is often offered as an intermediate step before considering injections.
If symptoms have not improved meaningfully after six to twelve weeks of consistent conservative management, it is reasonable to explore further options.
When Are Injections Appropriate for Plantar Fasciitis?
Injections are not a first resort, but they can be highly effective when conservative treatment has plateaued. At Joint Care London, we use ultrasound guidance for all plantar fascia injections, confirming accurate placement at the precise site of pathology. You can learn more about our approach to foot and ankle conditions and the range of procedures we offer.
Steroid vs PRP for Plantar Fasciitis: What Is the Difference?
Plantar Fasciitis Steroid Injection
A corticosteroid injection delivers a powerful anti-inflammatory agent directly into the affected area, and can reduce pain relatively quickly — often within one to two weeks. Steroid injections are most appropriate where there is a significant inflammatory component, typically in patients with symptoms of shorter duration.
An important consideration is the small but recognised risk of plantar fascia rupture and fat pad atrophy with repeated injections. For this reason, most clinicians recommend limiting corticosteroid injections to one or two in any twelve-month period, always delivered under ultrasound guidance.
PRP for Plantar Fasciitis
Platelet-rich plasma (PRP) is prepared from a small sample of your own blood, centrifuged to concentrate the platelets rich in growth factors for tissue repair. Rather than suppressing inflammation, PRP works by stimulating the body's natural healing response — making it particularly well-suited to chronic plantar fasciitis where tissue degeneration is the underlying problem.
PRP tends to work more gradually than steroid — patients typically begin to notice improvement at four to six weeks — but the effects are generally more sustained, with multiple studies showing durable improvements in pain scores at twelve months.
Choosing Between Steroid and PRP
- Steroid injection may be preferred for shorter-duration symptoms with an inflammatory component, or where rapid pain relief is a priority
- PRP is often the better choice for chronic or recurrent plantar fasciitis, or where steroid has previously provided only temporary benefit
What Does the Procedure Involve?
Both steroid and PRP injections for plantar fasciitis are performed as outpatient procedures and take around twenty to thirty minutes in total. All injections are performed under ultrasound guidance. After either procedure, you will be advised to keep weight off the foot for the remainder of the day.
Realistic Outcomes and Recovery
For steroid injections, studies report good short-term pain relief in the majority of patients, though a proportion experience recurrence within three to six months. PRP outcomes data for plantar fasciitis is encouraging, with multiple studies showing sustained improvements compared with both steroid and placebo at twelve months.
Neither treatment replaces the importance of addressing the underlying mechanical factors that contributed to the condition in the first place. Patients who engage with post-injection rehabilitation consistently achieve better results.
Tips to Prevent Recurrence
- Continue daily calf and plantar fascia stretching even when pain-free
- Invest in good footwear — avoid flat, unsupportive shoes
- Manage your activity load — increase running or training volume gradually
- Maintain a healthy weight — body weight directly affects load through the plantar fascia
- Address any biomechanical issues with a physiotherapist or podiatrist
- Act early if symptoms return — early intervention is significantly more straightforward than managing a chronic recurrence
Ready to Take the Next Step?
If you are dealing with persistent heel pain and conservative measures have not provided lasting relief, Joint Care London offers expert assessment and a full range of foot and ankle injection treatments including ultrasound-guided steroid injections and PRP therapy. To find out whether an injection-based treatment could be right for your plantar fasciitis, get in touch with our team to arrange a consultation.